Six things you should know about breast cancer risk
Six things you should know about breast cancer risk
There's no one big way to reduce your risk for breast cancer, but a combination of approaches could make a difference.
1. Weight gain
Many studies show that weight gain is a risk factor for breast cancer after menopause. An American Cancer Society study found that women who gained 20–30 pounds during adulthood (that is, after age 18) were 40% more likely to develop breast cancer after menopause than women who gained no more than 5 pounds. The link is estrogen, which is believed to promote the development of breast cancer. Fat tissue converts precursors in the body into estrogen, keeping the hormone in circulation even when ovarian production stops at menopause.
What to do?
Do all you can to avoid gaining weight as an adult, and try to enter menopause at a healthy weight. If you're overweight, try to lose weight.


2. Activity level
Many studies have shown that women who engage in regular physical activity have a lower risk of developing breast cancer compared with women who are sedentary. You may reduce your risk by 20%–30% by getting three to four hours of weekly exercise, from moderately intense (brisk walking and yoga, for example) to vigorous (such as jogging, cross-country skiing, and aerobic dance). Exercise also reduces the risk of recurrence if you have been treated for breast cancer.
What to do?
To reduce breast cancer risk, the American Cancer Society recommends moderate to vigorous activity for 45–60 minutes on at least five days of the week. (This is a step up from the 30 minutes of moderate activity most days of the week that's recommended for reducing chronic disease risk in adulthood.) Formal exercise (such as walking programs, swimming laps, cardio-fitness workouts, or aerobics classes) is a good way to get a sustained workout. But you can also do gardening activities or housework. — as long as you breathe as hard as you would during a brisk walk or jog.
3. Alcohol
Women who consume even a few drinks per week have an increased risk for breast cancer. Alcohol may raise estrogen levels, an important player in the development of breast cancer. It may interact with carcinogens or inhibit the body's capacity to detoxify them.
What to do?
Women at average risk for breast cancer should limit their intake of alcohol to one drink per day. Women who have had breast cancer or are at increased risk for it for other reasons may want to avoid alcohol altogether.


4. Vitamin D
Higher blood levels of vitamin D are associated with a lower risk of breast cancer compared to women with low levels of the vitamin. For example, one study found that women who got plenty of vitamin D in early life — either in their diet or by spending time outdoors, where sun exposure triggers vitamin D production in the skin — had a lower risk for breast cancer. Another investigation linked high blood levels of vitamin D with a 50% reduction in risk for breast cancer. Reaching those levels requires more than the recommended intake of 400 International Units (IU) of vitamin D per day for women ages 50–70.
What to do?
Experts have already begun to recommend 800–1,000 IU of vitamin D per day for adults, partly out of concern that we aren't getting enough of the vitamin from sunlight to protect our bones and partly because of its association with reduced cancer risk. Natural food sources of vitamin D are limited, and not everyone can get the amount of sunlight needed to trigger adequate vitamin D production in the skin. The best bet is supplemental vitamin D. A standard multivitamin usually supplies 400 IU; you can get an extra 400 IU in a vitamin D supplement.
5. Medication risks
Lifetime exposure to estrogen is a risk factor for breast cancer, so there is some concern about women's use of oral contraceptives and postmenopausal hormone therapy.
Women taking birth control pills are at a slightly increased risk of breast cancer, especially beyond the age of 35. The risk is significantly increased for women who take the pill and also smoke. However, in addition to preventing unwanted pregnancy, long-term use of oral contraceptives may also provide significant benefits in reducing your risk of ovarian, colon, and uterine cancers.
Still, for those at high-risk, or who are especially concerned about breast cancer prevention, avoiding birth control pills can help prevent the development of cancer.
What to do?
Birth control pills and hormone therapy have risks as well as benefits. Discuss them with your clinician before deciding whether to take them or for how long. If you know your mother took DES when she was pregnant with you, or if you took DES yourself, let your clinician know so you can discuss a screening schedule.

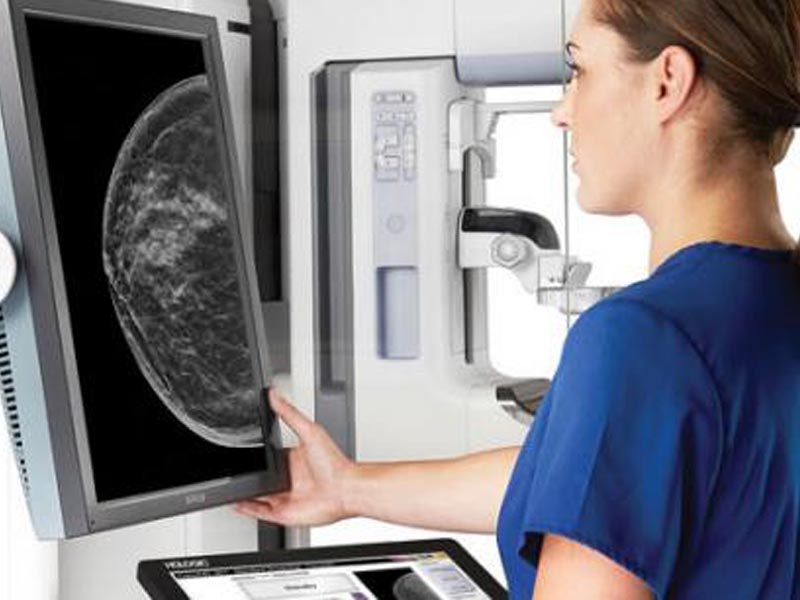
6. Breast density
Breasts are regarded as dense if they have less fat and more connective and glandular tissue. These features are more common in younger women's breasts, but they are also found in many older women, especially those taking combined hormone therapy (estrogen and progestin). Breast density is also partly a heritable trait.
Women with dense breasts are at increased risk for breast cancer.
What to do?
Unfortunately, breast tumors (both cancerous and noncancerous) can be difficult to distinguish against a background of dense breast tissue on a mammogram. That's because tumors and dense tissue appear white; fatty tissue, on the other hand, looks darker and provides a contrast to the tumors. Digital mammography has been shown to improve cancer detection in women with dense breasts, because it allows the radiologist to fine-tune images so that tiny abnormalities stand out better. Ultrasound or MRI can also help answer questions raised by a suspicious mammogram. Much more needs to be learned about breast density before official recommendations can be made. In the meantime, if you have dense breasts, talk to your clinician about screening with digital mammography.


