DESERT IMAGINGVARICOSE VEINS
Understanding Venous Reflux Disease
Varicose veins or spider veins can be a cause for concern – whether because of their appearance or the discomfort they can cause. Healthy leg veins contain valves that open and close, helping push blood back to the heart after it circulates throughout the body. But when varicose veins start to form, it can be a sign that those valves have become damaged or diseased, causing blood to pool in your legs. This is called venous reflux disease. We typically see these conditions in older adults, but other risk factors include obesity, hormone changes due to pregnancy or menopause, and spending extended amounts of time standing. For this reason, people who work in nursing, teaching, or factory settings frequently develop venous reflux.
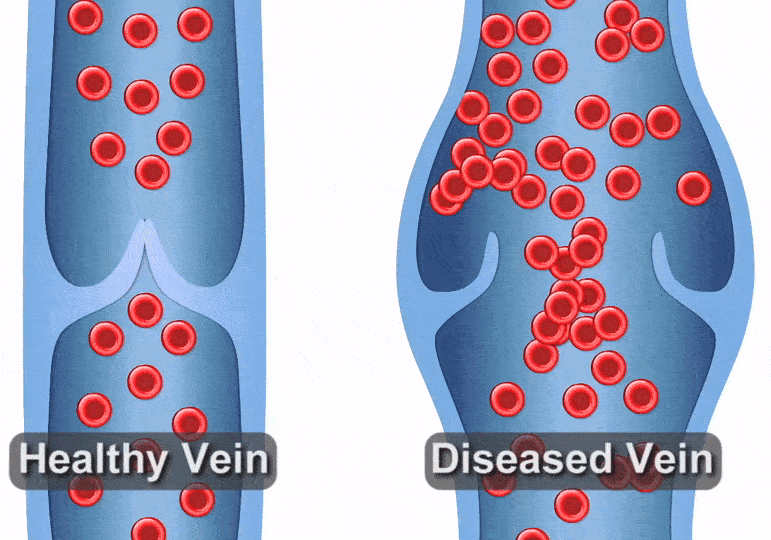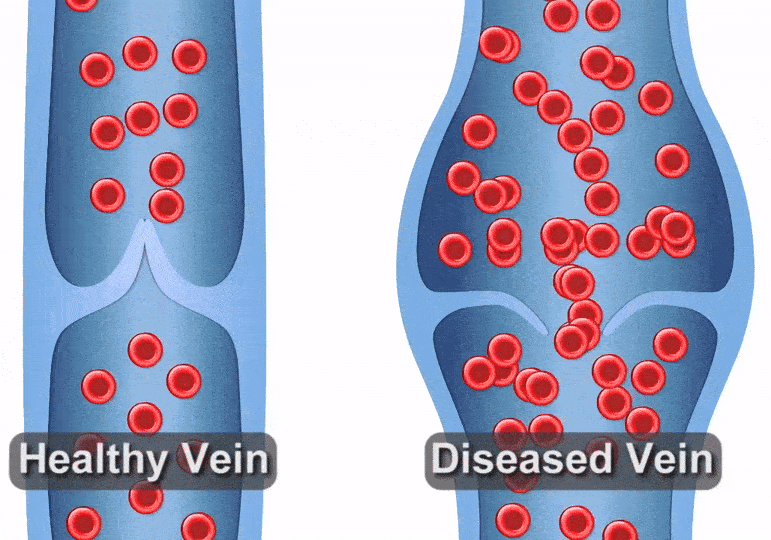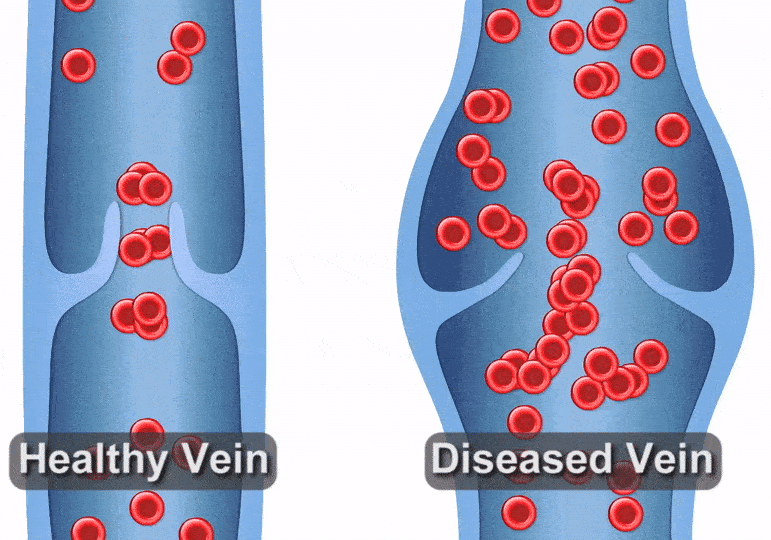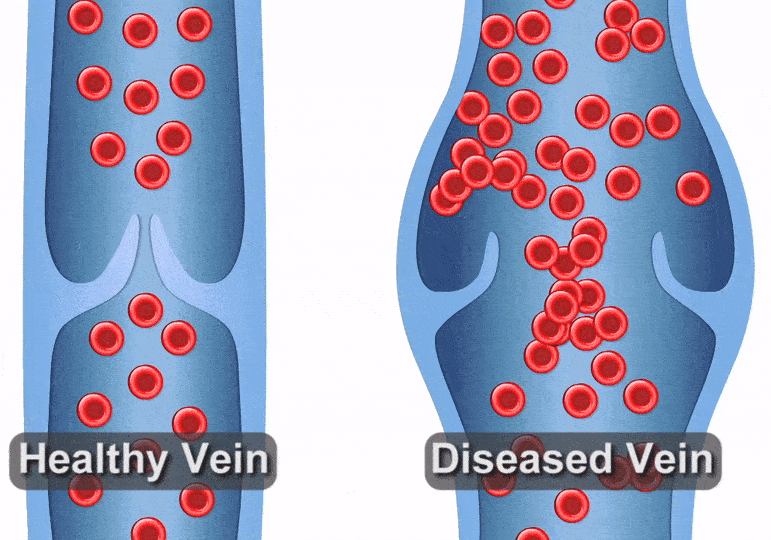
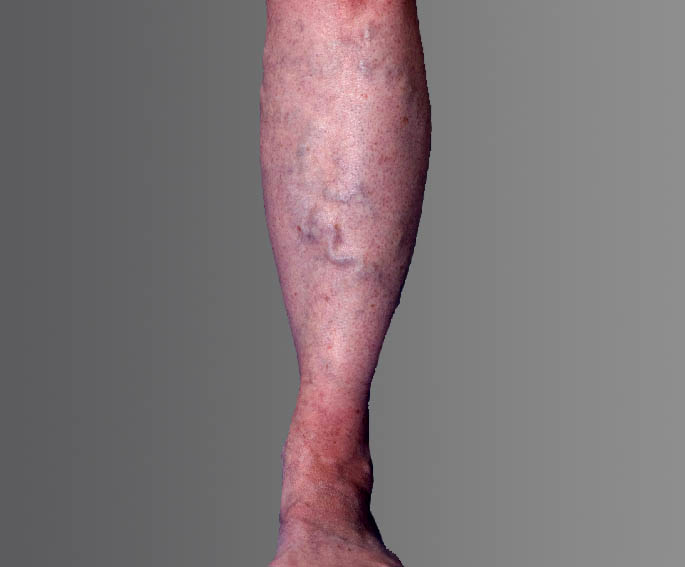
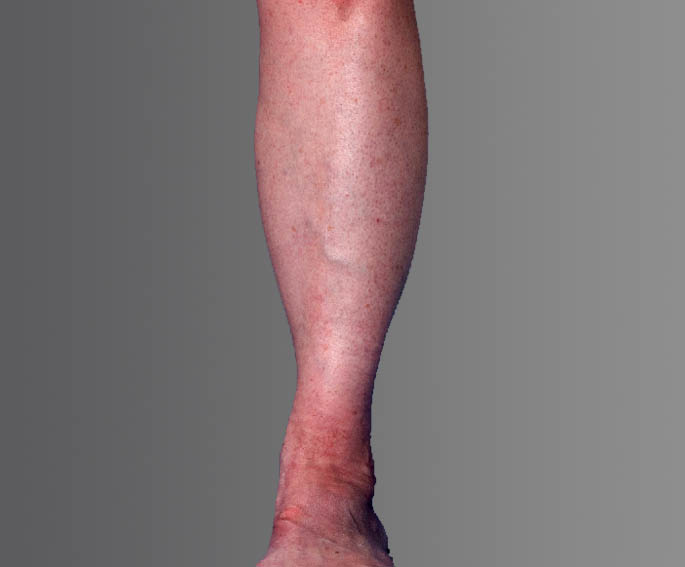
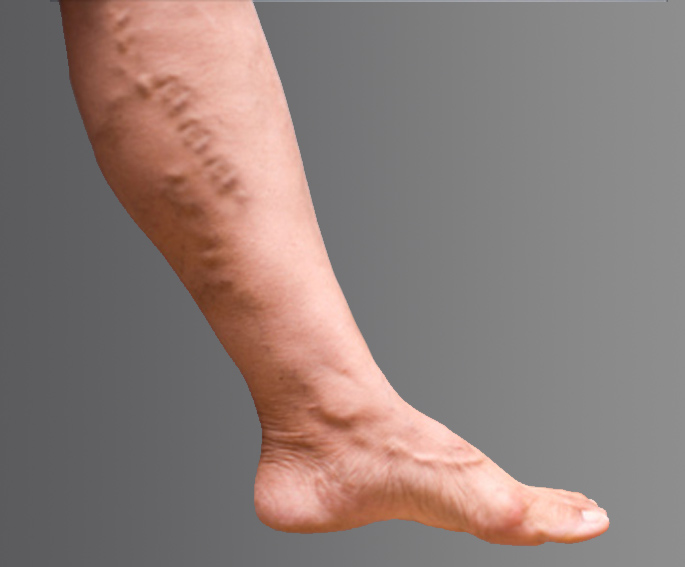
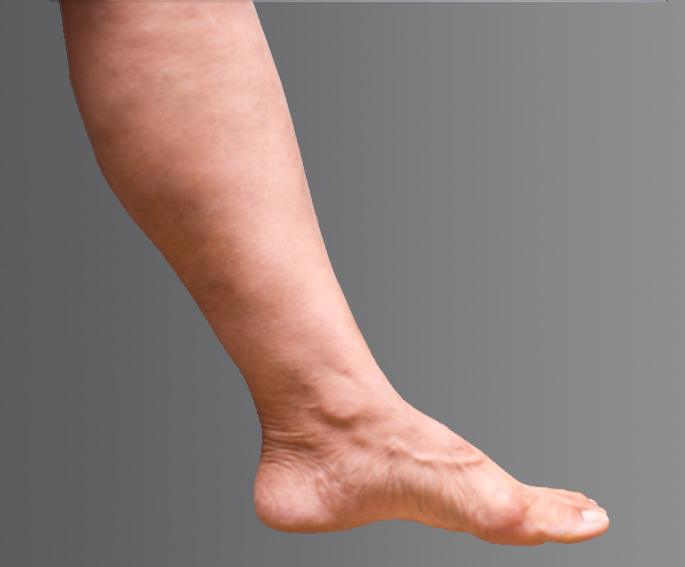
Venous reflux can create a host of problems, but people often notice the visual effects first – unsightly veins forming on the legs. Varicose veins in the leg may become thick, dark, and enlarged, whereas spider veins are typically smaller and flatter, but may be a darker red to blue color. This visual sign is often a signal that you may be at risk for other complications, such as pain while walking, standing, or moving throughout the day. You may also experience an uncomfortable heavy feeling in the legs, pain that gets worse when you stand, weakness, itching, swelling, aching, and even throbbing. Left untreated, venous reflux can cause these problems to get worse or can increase the risk of blood clots.

Treatment for venous reflux can vary quite a bit, depending on the patient and the severity of the condition.
In some cases, varicose veins can be treated with prescription medication or by wearing compression stockings for a period of time, typically four to eight weeks.
Extreme conditions may require surgery, but interventional radiology can often provide the same results with minimal risk to the patient.
Interventional radiology uses guided imaging
to locate the damaged blood valves and determine whether they can be fixed or need to be removed. Once imaging provides a clear idea of the problem, doctors can apply therapy within the vein using fine needles or a catheter, using a local anesthetic. These procedures are far less invasive than normal surgery and can be performed on an outpatient basis. Patients typically report little to no pain during the procedure. Because it is minimally invasive, there is also minimized bruising, fewer complications, and a shorter recovery time.
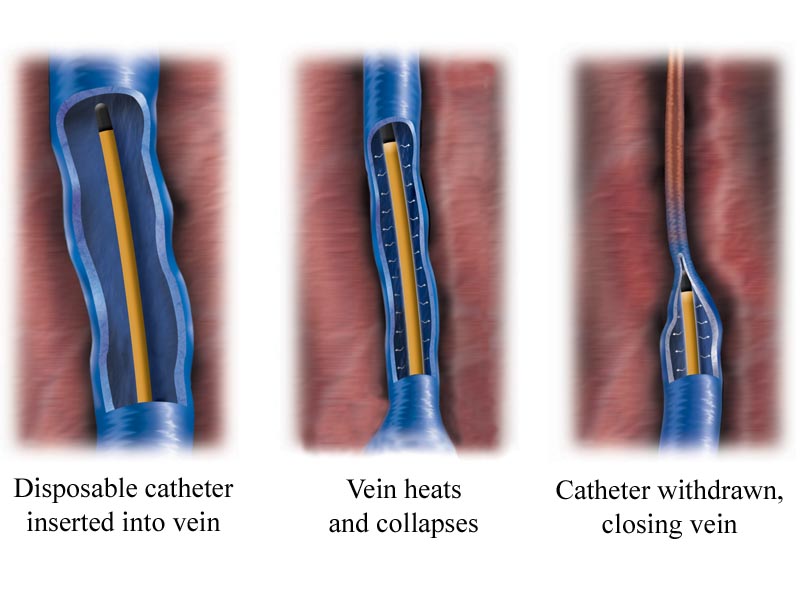
Visual Results
The average patient typically resumes normal activities within a few days.*Individual results may vary